Hospice Information Session January 29 2026

[et_pb_section admin_label=”section”] [et_pb_row admin_label=”row”] [et_pb_column type=”4_4″][et_pb_text admin_label=”Text”] End of Life Choices California is a nonprofit organization that offers trained client volunteers to work with Californians who are seriously or terminally […]
Hospice Information Session January 29 2026

[et_pb_section admin_label=”section”] [et_pb_row admin_label=”row”] [et_pb_column type=”4_4″][et_pb_text admin_label=”Text”] End of Life Choices California is a nonprofit organization that offers trained client volunteers to work with Californians who are seriously or terminally […]
Golden Future Senior Expo – San Diego Edition

The Golden Future Senior Expo – San Diego Edition is celebrating its 15th year and will host a large variety of exhibitions presenting valuable information and resources for seniors and […]
Golden Future Senior Expo – San Diego Edition

The Golden Future Senior Expo – San Diego Edition is celebrating its 15th year and will host a large variety of exhibitions presenting valuable information and resources for seniors and […]
Aging Forward Expo Santa Rosa

Join us for a community event dedicated to empowering adults 50+ to plan for a vibrant, healthy, and secure future. The Expo features trusted local organizations, resources, and handmade crafts. […]
Aging Forward Expo Santa Rosa

Join us for a community event dedicated to empowering adults 50+ to plan for a vibrant, healthy, and secure future. The Expo features trusted local organizations, resources, and handmade crafts. […]
Senior Expo of Santa Barbara

The Senior Expo of Santa Barbara will have 100+ exhibitions presenting valuable information and resources for seniors and their caregivers. Find us at EOLCCA’s booth where our knowledgeable Volunteers will answer […]
Senior Expo of Santa Barbara

The Senior Expo of Santa Barbara will have 100+ exhibitions presenting valuable information and resources for seniors and their caregivers. Find us at EOLCCA’s booth where our knowledgeable Volunteers will answer […]
Hospice Information Session

End of Life Choices California is a nonprofit organization that offers trained client volunteers to work with Californians who are seriously or terminally ill, or those simply thinking ahead and […]
Hospice Information Session

End of Life Choices California is a nonprofit organization that offers trained client volunteers to work with Californians who are seriously or terminally ill, or those simply thinking ahead and […]
Brookdale: Advance Care Planning and End of Life Options

California End of Life Option Act Presenters: Mark H. Greenberg, Executive Director, and Reina Galanes, Speaker’s Program Coordinator with End of Life Choices California (EOLCCA), will discuss the importance of […]
Brookdale: Advance Care Planning and End of Life Options

California End of Life Option Act Presenters: Mark H. Greenberg, Executive Director, and Reina Galanes, Speaker’s Program Coordinator with End of Life Choices California (EOLCCA), will discuss the importance of […]
Brookdale: Advance Care Planning and End of Life Options

California End of Life Option Act Presenters: Mark H. Greenberg, Executive Director, and Reina Galanes, Speaker’s Program Coordinator with End of Life Choices California (EOLCCA), will discuss the importance of […]
Abrazar: Information & Support for End-of-Life Planning

[et_pb_section fb_built=”1″ _builder_version=”4.27.0″ global_colors_info=”{}”][et_pb_row _builder_version=”4.27.0″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”][et_pb_column type=”4_4″ _builder_version=”4.16″ custom_padding=”|||” global_colors_info=”{}” custom_padding__hover=”|||”][et_pb_text _builder_version=”4.27.0″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”] This presentation will help Abrazar’s staff to discuss end-of-life planning in […]
Abrazar: Information & Support for End-of-Life Planning

[et_pb_section fb_built=”1″ _builder_version=”4.27.0″ global_colors_info=”{}”][et_pb_row _builder_version=”4.27.0″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”][et_pb_column type=”4_4″ _builder_version=”4.16″ custom_padding=”|||” global_colors_info=”{}” custom_padding__hover=”|||”][et_pb_text _builder_version=”4.27.0″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”] This presentation will help Abrazar’s staff to discuss end-of-life planning in […]
Abrazar: Information & Support for End-of-Life Planning

[et_pb_section fb_built=”1″ _builder_version=”4.27.0″ global_colors_info=”{}”][et_pb_row _builder_version=”4.27.0″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”][et_pb_column type=”4_4″ _builder_version=”4.16″ custom_padding=”|||” global_colors_info=”{}” custom_padding__hover=”|||”][et_pb_text _builder_version=”4.27.0″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”] This presentation will help Abrazar’s staff to discuss end-of-life planning in […]
Senior Center in Central Park: End of Life Options In California

[et_pb_section fb_built=”1″ _builder_version=”4.16″ global_colors_info=”{}”][et_pb_row _builder_version=”4.16″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”][et_pb_column type=”4_4″ _builder_version=”4.16″ custom_padding=”|||” global_colors_info=”{}” custom_padding__hover=”|||”][et_pb_text _builder_version=”4.27.0″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”] A discussion of end-of-life options and the right to medical aid […]
Senior Center in Central Park: End of Life Options In California

[et_pb_section fb_built=”1″ _builder_version=”4.16″ global_colors_info=”{}”][et_pb_row _builder_version=”4.16″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”][et_pb_column type=”4_4″ _builder_version=”4.16″ custom_padding=”|||” global_colors_info=”{}” custom_padding__hover=”|||”][et_pb_text _builder_version=”4.27.0″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”] A discussion of end-of-life options and the right to medical aid […]
Senior Center in Central Park: End of Life Options In California

[et_pb_section fb_built=”1″ _builder_version=”4.16″ global_colors_info=”{}”][et_pb_row _builder_version=”4.16″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”][et_pb_column type=”4_4″ _builder_version=”4.16″ custom_padding=”|||” global_colors_info=”{}” custom_padding__hover=”|||”][et_pb_text _builder_version=”4.27.0″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”] A discussion of end-of-life options and the right to medical aid […]
Piedmont Gardens: End of Life Options in California

[et_pb_section fb_built=”1″ admin_label=”section” _builder_version=”4.16″ global_colors_info=”{}”][et_pb_row admin_label=”row” _builder_version=”4.16″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”][et_pb_column type=”4_4″ _builder_version=”4.16″ custom_padding=”|||” global_colors_info=”{}” custom_padding__hover=”|||”][et_pb_text admin_label=”Text” _builder_version=”4.26.0″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”] Legal end-of-life options in California include discontinuing or […]
Piedmont Gardens: End of Life Options in California

[et_pb_section fb_built=”1″ admin_label=”section” _builder_version=”4.16″ global_colors_info=”{}”][et_pb_row admin_label=”row” _builder_version=”4.16″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”][et_pb_column type=”4_4″ _builder_version=”4.16″ custom_padding=”|||” global_colors_info=”{}” custom_padding__hover=”|||”][et_pb_text admin_label=”Text” _builder_version=”4.26.0″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”] Legal end-of-life options in California include discontinuing or […]
Piedmont Gardens: End of Life Options in California

[et_pb_section fb_built=”1″ admin_label=”section” _builder_version=”4.16″ global_colors_info=”{}”][et_pb_row admin_label=”row” _builder_version=”4.16″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”][et_pb_column type=”4_4″ _builder_version=”4.16″ custom_padding=”|||” global_colors_info=”{}” custom_padding__hover=”|||”][et_pb_text admin_label=”Text” _builder_version=”4.26.0″ background_size=”initial” background_position=”top_left” background_repeat=”repeat” global_colors_info=”{}”] Legal end-of-life options in California include discontinuing or […]
Looking for answers about the use of MAiD

Know that in California medical aid in dying is available to you. You may never need it, but you have the right to understand it and choose it if the time comes.
The Sequoias San Francisco

This event is sponsored by The Sequoias’ HELP – honoring end of life preferences’ Committee.
The Sequoias San Francisco

This event is sponsored by The Sequoias’ HELP – honoring end of life preferences’ Committee.
The Sequoias San Francisco

This event is sponsored by The Sequoias’ HELP – honoring end of life preferences’ Committee.
Temple Beth Hillel, Valley Village

Screening of “Last Flight Home” followed by Q&A discussion led by Rabbi Suzanne Singer and Joyce Mayne.
Temple Beth Hillel, Valley Village

Screening of “Last Flight Home” followed by Q&A discussion led by Rabbi Suzanne Singer and Joyce Mayne.
Temple Beth Hillel, Valley Village

Screening of “Last Flight Home” followed by Q&A discussion led by Rabbi Suzanne Singer and Joyce Mayne.
Golden Gate Village at the Richmond Senior Center

A discussion about end-of-life choices and the right to medical aid in dying in California.
Golden Gate Village at the Richmond Senior Center

A discussion about end-of-life choices and the right to medical aid in dying in California.
Golden Gate Village at the Richmond Senior Center

A discussion about end-of-life choices and the right to medical aid in dying in California.
Villa Marin Retirement Community

A discussion about end-of-life options and the right to medical aid in dying in California.
Villa Marin Retirement Community

A discussion about end-of-life options and the right to medical aid in dying in California.
Villa Marin Retirement Community

A discussion about end-of-life options and the right to medical aid in dying in California.
Hope Hospice Sun City,CA

Providing information to key personnel at Hope Hospice & Health Care as to their internal policies and procedures supporting patients who inquire about or choose to utilize the California End of Life Option Act for medical aid in dying.
Hope Hospice Sun City,CA

Providing information to key personnel at Hope Hospice & Health Care as to their internal policies and procedures supporting patients who inquire about or choose to utilize the California End of Life Option Act for medical aid in dying.
Hope Hospice Sun City,CA

Providing information to key personnel at Hope Hospice & Health Care as to their internal policies and procedures supporting patients who inquire about or choose to utilize the California End of Life Option Act for medical aid in dying.
Marin Villages at San Rafael

California’s Medical Aid in Dying Act is not well-known.
Marin Villages at San Rafael

California’s Medical Aid in Dying Act is not well-known.
Marin Villages at San Rafael

California’s Medical Aid in Dying Act is not well-known.
New MAiD Study shows gap in public awareness and institutional support
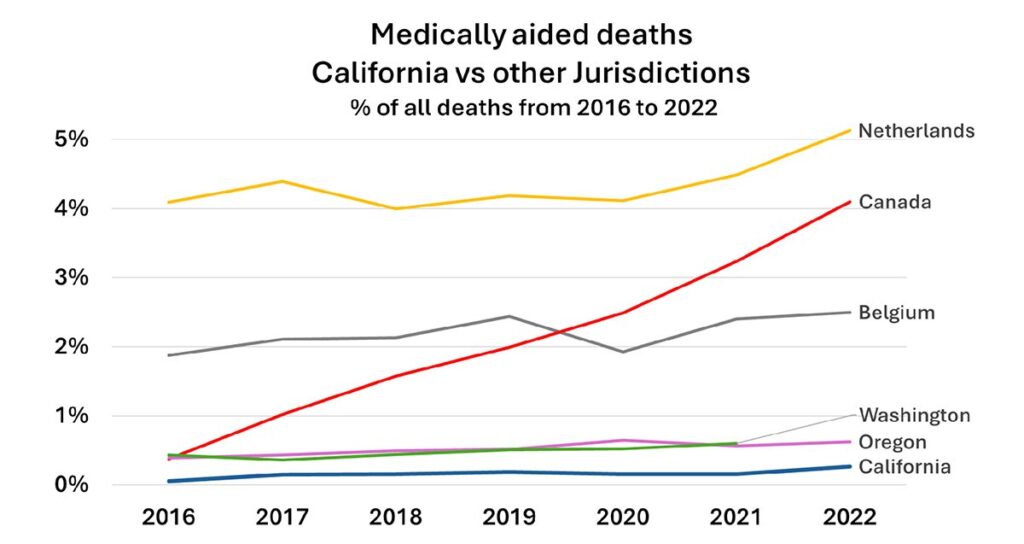
Californians nearly 16 times less likely than Canadians to choose Medical Aid in Dying
New MAiD Study shows gap in public awareness and institutional support

Californians nearly 16 times less likely than Canadians to choose Medical Aid in Dying
New MAiD Study shows gap in public awareness and institutional support

Californians nearly 16 times less likely than Canadians to choose Medical Aid in Dying
New Study Shows Only a Quarter of Californians Are Aware of Medical Aid in Dying Rights

End of Life Choices California Board Director Adrian Byram co-authors study evaluating disparities in public awareness and institutional support from healthcare systems and found that Californians are nearly 16 times less likely than Canadians to choose Medical Aid in Dying.
Jackie Robinson Family YMCA Health Fair San Diego 6.5.24

Be sure to visit the End of Life Choices California (EOLCCA) information booth at this excellent YMCA health fair offered in San Diego.
Jackie Robinson Family YMCA Health Fair San Diego 6.5.24

Be sure to visit the End of Life Choices California (EOLCCA) information booth at this excellent YMCA health fair offered in San Diego.
Jackie Robinson Family YMCA Health Fair San Diego 6.5.24

Be sure to visit the End of Life Choices California (EOLCCA) information booth at this excellent YMCA health fair offered in San Diego.
Jackie Robinson Family YMCA Health Fair 5.1.24

Be sure to visit the End of Life Choices California (EOLCCA) information booth at this excellent YMCA health fair offered in San Diego.
Jackie Robinson Family YMCA Health Fair 5.1.24

Be sure to visit the End of Life Choices California (EOLCCA) information booth at this excellent YMCA health fair offered in San Diego.
